Retinal Conditions

Central serous retinopathy (CSR), also known as central serous chorioretinopathy (CSC), is a visual impairment, often temporary, usually in one eye, mostly affecting males in the age group 20 to 50 but which may also affect women. The disorder is characterized by leakage of fluid in the central macula, which results in blurred or distorted vision (metamorphopsia). A blind or gray spot in the central vision is common, along with flashes of light (photopsia).
Causes
CSR is a fluid detachment of macula layers from their supporting tissue. This allows choroidal fluid to leak into the subretinal space. The build up of fluid seems to occur because of small breaks in the retinal pigment epithelium. CSR is sometimes called idiopathic CSR which means that its cause is unknown. Nevertheless, stress appears to play an important role.
CSR has also been associated with cortisol and corticosteroids, and persons with higher levels of cortisol than normal also have a higher propensity to suffer from CSR
Treatment
There is no known effective treatment for the disease. Laser photocoagulation, which effectively burns the leak area shut, is sometimes suggested. In many cases the leak is very near the central macula, where photocoagulation would leave a blind spot. Additionally, a better long term outcome has not been demonstrated with photocoagulation. So, more often than not, the condition goes untreated.
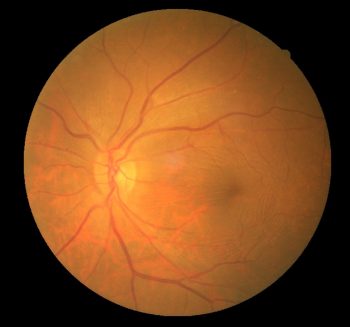

Epiretinal membrane is also known as macular pucker. It is a thin sheet of fibrous tissue that can develop on the surface of the macular area of the retina.
The macula normally lies flat against the back of the eye, like film lining the back of a camera. When wrinkles, creases or bulges form on the macula, this is known as epiretinal membrane.
Due to ageing, the vitreous gel (clear, gel-like substance) in the eye begins to shrink and pull away from the retina. As the vitreous pulls away, scar tissue may develop on the macula. The scar tissue can warp and contract and cause the retina to wrinkle or bulge.
SymptomsMost epiretinal membranes are mild and have little or no effect on vision. However, in some cases, the epiretinal membrane may slowly grow and begin to cause mechanical distortion (“wrinkling”) in the macula. This may lead to blurred or distorted vision, which may slowly worsen over time.
TreatmentFor mild epiretinal membrane, no treatment is necessary. Changing glasses prescription may improve vision sometimes. Eyedrops, medicines or laser surgery do not improve vision.
The retina is the layer of tissue at the back of the inner eye that converts light images to nerve signals and sends them to the brain. Retinal vein occlusion is a blockage of the small veins that carry blood away from the retina. Haemorrhages (bleeding) and leakage of fluid can occur from the areas of blockage.
Types of Retinal Vein Occlusion
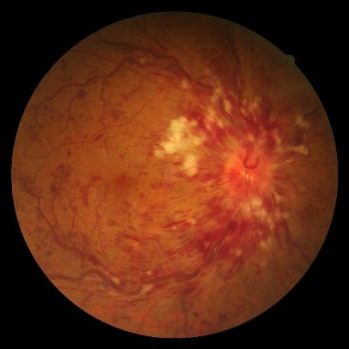
1. Central retinal vein occlusion (CRVO): Blockage at main vein of the eye located at optic nerve
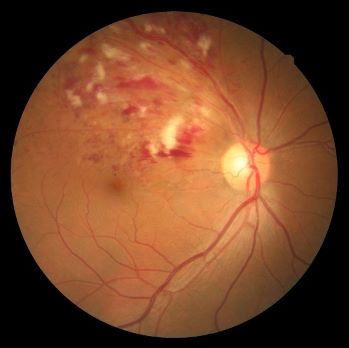
2. Branch retinal vein occlusion (BRVO): Blockage at one of the smaller branches of vessels attached to the main vein
Retinal vein occlusion is most often caused by hardening of the arteries (atherosclerosis) and the formation of a blood clot.
SymptomsCRVO is associated with painless unilateral (one eye) loss of vision. In some cases, this loss of vision is subtle in character, with intermittent episodes of blurred vision. In other cases, it may be sudden and dramatic.
BRVO is often noted with an onset of blurred vision or visual field defect. Vision loss may be subtle. Patients with small occlusions of a branch retinal vein may often be asymptomatic.
Treatment
Many people will regain vision, even without treatment. However, vision rarely returns to normal. There is no way to reverse or open the blockage.
In some cases, treatment for the complications of retinal vein occlusion may be given including:
- Intraocular injections of anti-vascular endothelial growth factor (anti-VEGF) drugs into the eye. These drugs may block the growth of new blood vessels that can cause glaucoma. This treatment is still being studied.
- Focal laser treatment to treat macular edema
- Laser treatment to prevent the growth of new, abnormal blood vessels (neovascularisation) that leads to glaucoma
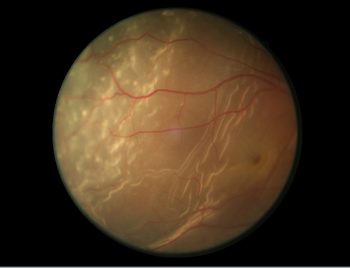

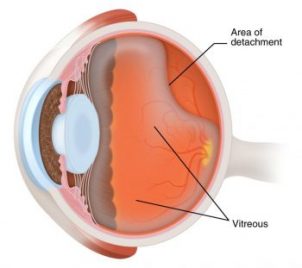
Retinal detachment is when the retina is pulled away from its normal position and separated from the underlying tissues within the eye. The retina will not be able to function normally and blurring of vision will occur. A retinal detachment can progress and result in total retinal detachment, affecting the whole retina.
Causes1. Posterior Vitreous Detachment is an ageing process. The vitreous, a jelly-like substance which gives our eye its shape, shrinks and liquefies causing the vitreous to pull away from the retina. Traction occurs as a result when the vitreous pulls and tugs onto the retina and flashes of light might be noticed at the peripheral of your vision. This could create holes or tears on the retina.
2. Retinal holes and tears are usually caused by posterior vitreous detachment. If treatment is not carried out, fluid from the vitreous will enter these holes or tears accumulating behind the retina. Build-up of fluid behind the retina separates and causes a retinal detachment.
Risks of retinal detachment- Myopia
- Serious trauma or injury to the eye or head
- Previous history of retinal detachment in other eye
- Family history of retinal detachment
- Weak areas in the retina
- New floaters
- Flashes of lights
- A shadow noted at the side of your vision
- Sudden blurring of vision
- Argon Laser Argon laser treatment is carried out if there are holes or tears in the retina. The laser would be applied around these holes or tears. Scar tissue will be formed around the retinal tear or hole sealing it to prevent fluid from entering them and causing a retinal detachment.
- Scleral Buckling Scleral buckling treatment is carried out by having a band made out of silicone or plastic around the outer wall of the eye acting as a belt, pressing the eye so that the retinal hole or tear is pushed against the wall of the eye. The surgeon usually drains out the fluid that is behind the retina, allowing the retina to flatten back into place.
- Pneumatic Retinopexy A gas bubble is injected directly into the vitreous cavity inside the eye. The gas bubble will push the retina against the back of the eye, placing it back in its position.
- Vitrectomy Vitrectomy is usually carried out if there is traction when the vitreous is pulling on the retina or when there is bleeding in the vitreous. The jelly of the eye will be removed and replaced, removing this traction in the eye. Scleral buckling may be performed together with vitrectomy.
Symptoms
Treatment
1. Retinal Holes or Tears Surgery
2. Retinal Detachment Surgery
Laser treatment may be carried out before this procedure.
Laser treatment may be carried out before this procedure.




 BACK
BACK